It’s common for patients in need of critical care to experience some loss of muscle strength during their stay in an intensive care unit (ICU). Unfortunately, even if the patient was strong and mobile before their illness or injury, this can cause long-term issues with weakness and mobility.
“Most patients who are critically ill tend to lose a lot of muscle mass just from being in bed,” says Dr. John Muscedere, a clinician-scientist at KHSC’s Kingston General Hospital (KGH) site. “It’s increasingly recognized that mobility for patients in the ICU is important. The more you mobilize patients, the better their outcomes.”
But how can we effectively maintain muscle strength in patients who are sedated and being supported by a ventilator? This question is what inspired Dr. Michelle Kho of McMaster University to design the CYCLE (Critical care cYCling to improve Lower Extremity strength) research program, which provides hospital sites with a specially designed cycling machine to aid in delivering physiotherapy to critical care patients.
“People who were able to walk before their illness are at risk of having trouble walking even five years after their ICU stay,” says Dr.Kho, during a visit to KHSC’s Kingston General Hospital (KGH) site. “If we can start to target this population with cycling therapy early in their stay, we believe it will help them speed up their recovery.”
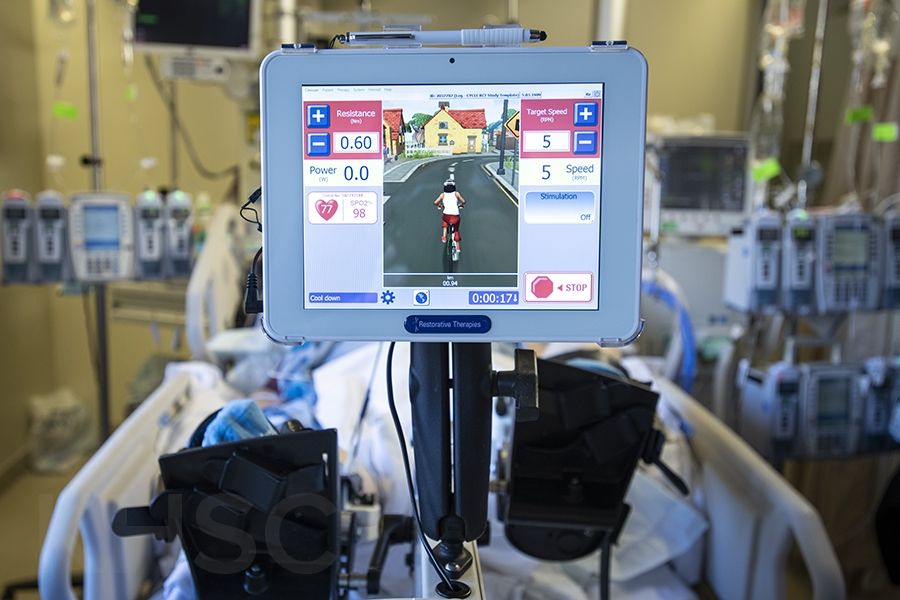
The custom-made recumbent cycle has straps to secure patients’ feet into moving pedals. As they lay in bed, the patient will either be passively cycling with the support of the machine or actively cycling using their own strength and energy, depending on their level of sedation.
Eligible participants will cycle for 30 minutes up to five days a week during their stay. These results will be compared against a group of patients who undergo more traditional methods of mobility such as range of motion movements to prevent stiff muscles, or walking around their room with assistance.
“This is an extra way for patients to get more exercise and move their muscles while they are still in bed, before they may be able to stand or walk,” explains Dr. Muscedere. “With this technology, we can start physiotherapy and rehabilitative activity much earlier.”
The success of the CYCLE program relies on the collaboration of critical care nurses, physiotherapists, physicians and researchers from around the world to identify eligible participants and collect data.
“We are really happy to be a part of this study,” says Dr. Muscedere. “We have been involved in its design for a while so it’s great to get it up and going. I’m grateful for all the support from the physiotherapy staff, nurses, and the hospital administration. It’s a true team effort.”
For more information about the CYCLE study, visit icucycle.com.
Gallery
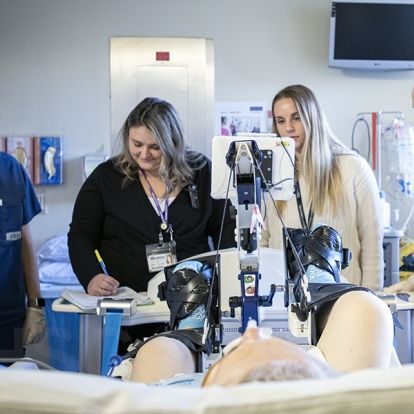
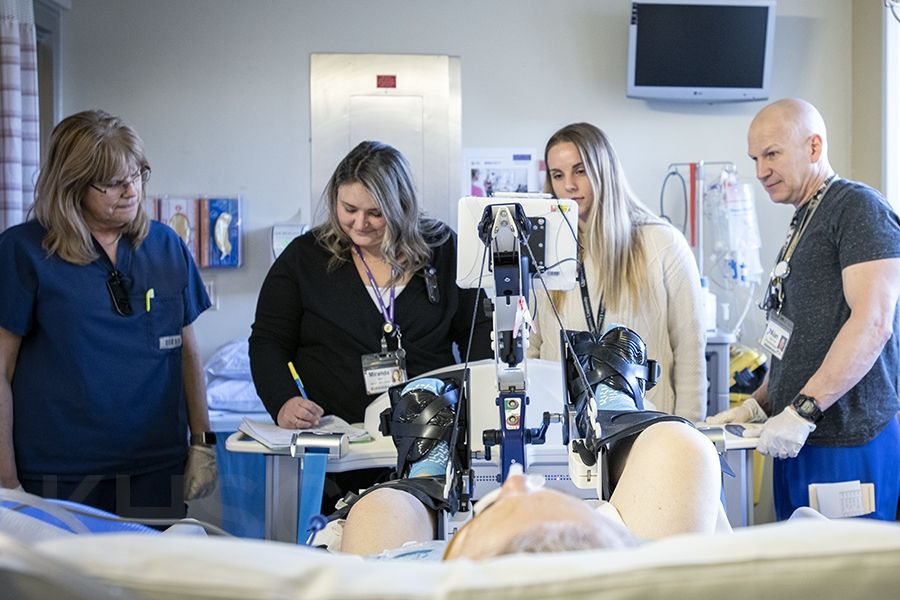
A team of multi-disciplinary staff monitoring a patient participating in the CYCLE research program.
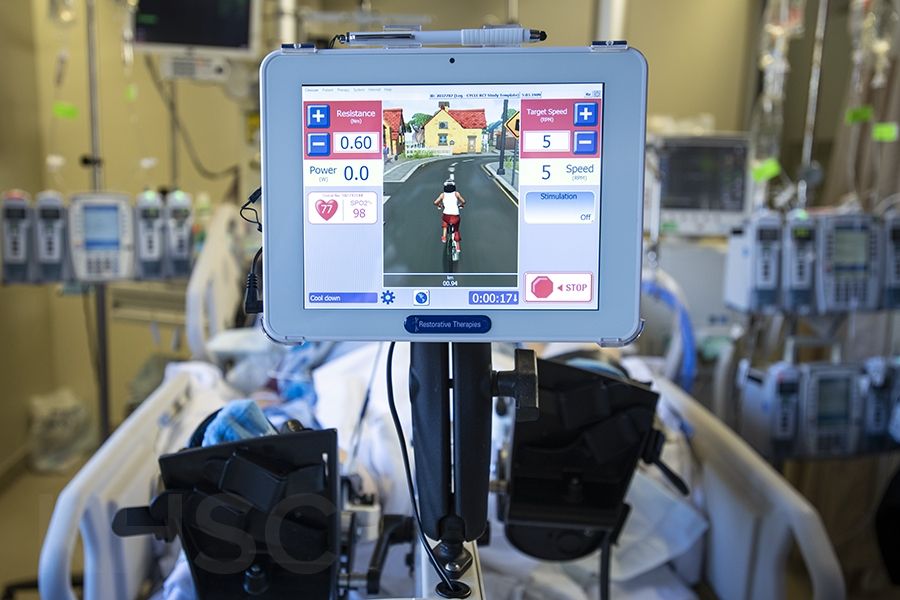
Patients will use a specialized cycle during their ICU stay to maintain muscle mass and increase long-term outcomes in their mobility.



