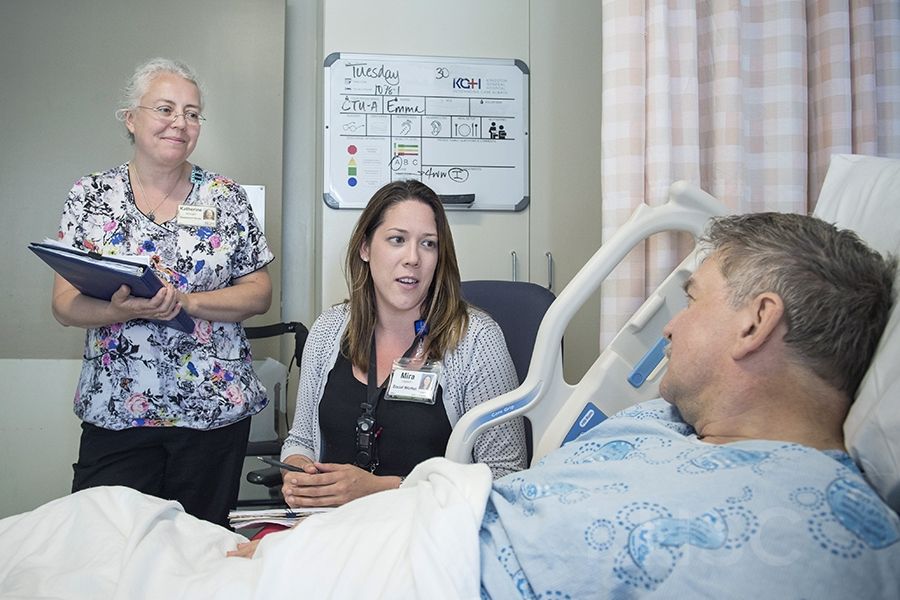
An innovative pilot program between Bayshore HealthCare and Kingston Health Sciences Centre (KHSC) has received funding to operate for a second year after demonstrating improved outcomes for patients who are transitioning out of the hospital and back into their own homes.
The Alternative Level of Care (ALC) Transitional Care Unit, operated by Bayshore HealthCare, was extremely successful in its first year as it was able to decrease the amount of time ALC patients remained in the hospital, allowing them to transition to a more appropriate environment based on their needs. It is a 10 bed unit, located in a retirement home, which serves patients who still require support, but no longer need the complex care provided by KHSC.
“This program is designed for patients whose hospital care plan is complete, but who are unable to return to their pre-hospital living arrangement,” explains Silvie Crawford, Executive Vice-President and Chief Nursing Executive at KHSC. “The majority of patients that require ALC are seniors and just need some extra support and care before they are ready to go home. By partnering with Bayshore, we can ensure they receive the care they need in a setting that is more suited to their specific needs. We are grateful to the South East Local Health Integration Network and the Ministry of Health and Long Term Care for their support of this initiative.”
By receiving care in the ALC Transitional Care Unit, eligible patients have access to many restorative therapies as well as nursing and personal care support to help them prepare for life at home again. This environment also provides time for patients and their family to receive additional education on how best to care for themselves after discharge.
“Programs like this one enhance the recovery process by helping patients regain their strength and independence,” says Karen Fisher, Director of Community Partnerships at Bayshore HealthCare. “We work collaboratively with patients, families and caregivers to prepare patients for their transition back into their homes, and so far we have had wonderful results.”
The goal of the pilot program was to have patients receiving care on the transition unit for 45 to 60 days, but caregivers found that the average patient was ready to transition out of the program after only 33 days. Many times patients transitioned back into their own homes, but sometimes patients chose to transition into a retirement community instead.
“We were very pleased with the success of this model,” says Tom Hart, Director of Patient Access, Flow and Clinical Resources with KHSC. “Partnerships like this one support patients and families by transitioning ALC patients into a specialized community setting, while also creating additional capacity at KHSC for the sickest patients in the region that need our care.”
“If the program continues to perform well, it has potential to be used as a model for other cities to adapt and help improve wait-times for ALC care across our region and the province,” adds Crawford.
More than 95 patients have been cared for through the pilot program, adding up to over 2400 days of hospital beds being made available for patients who required a higher level of care. By having more bed days available, patients in need of hospital care may experience shorter wait-times for a bed.
“Programs like this one demonstrate how important it is for our community healthcare services to be partners,” says Anita Fitches, Director, Integrated Care Solutions at Bayshore HealthCare. “We are excited that we can continue working together to find ways to improve care for the people of our community and beyond.”
Gallery

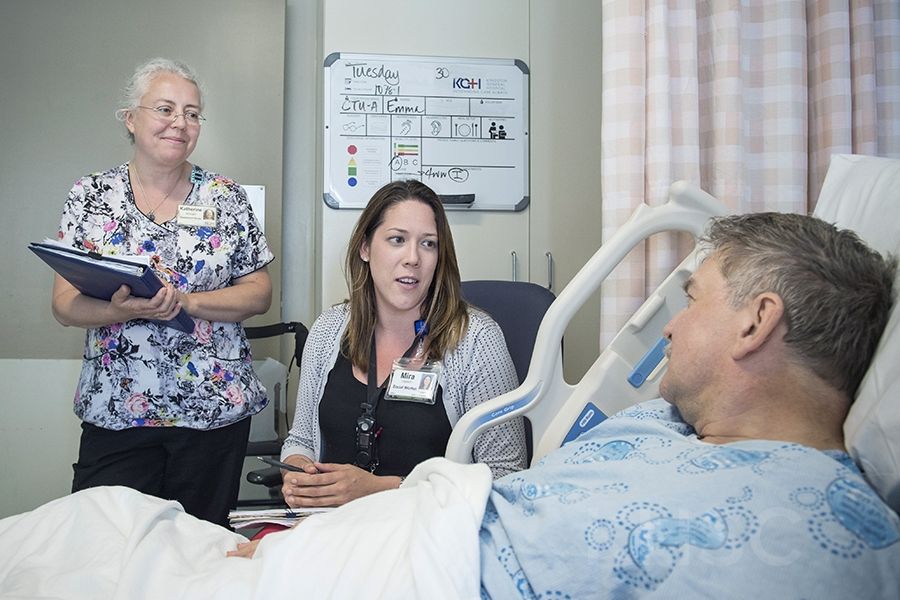
The project allows patients designated as needing an alternate level of care to transition out of the hospital to a more appropriate environment



